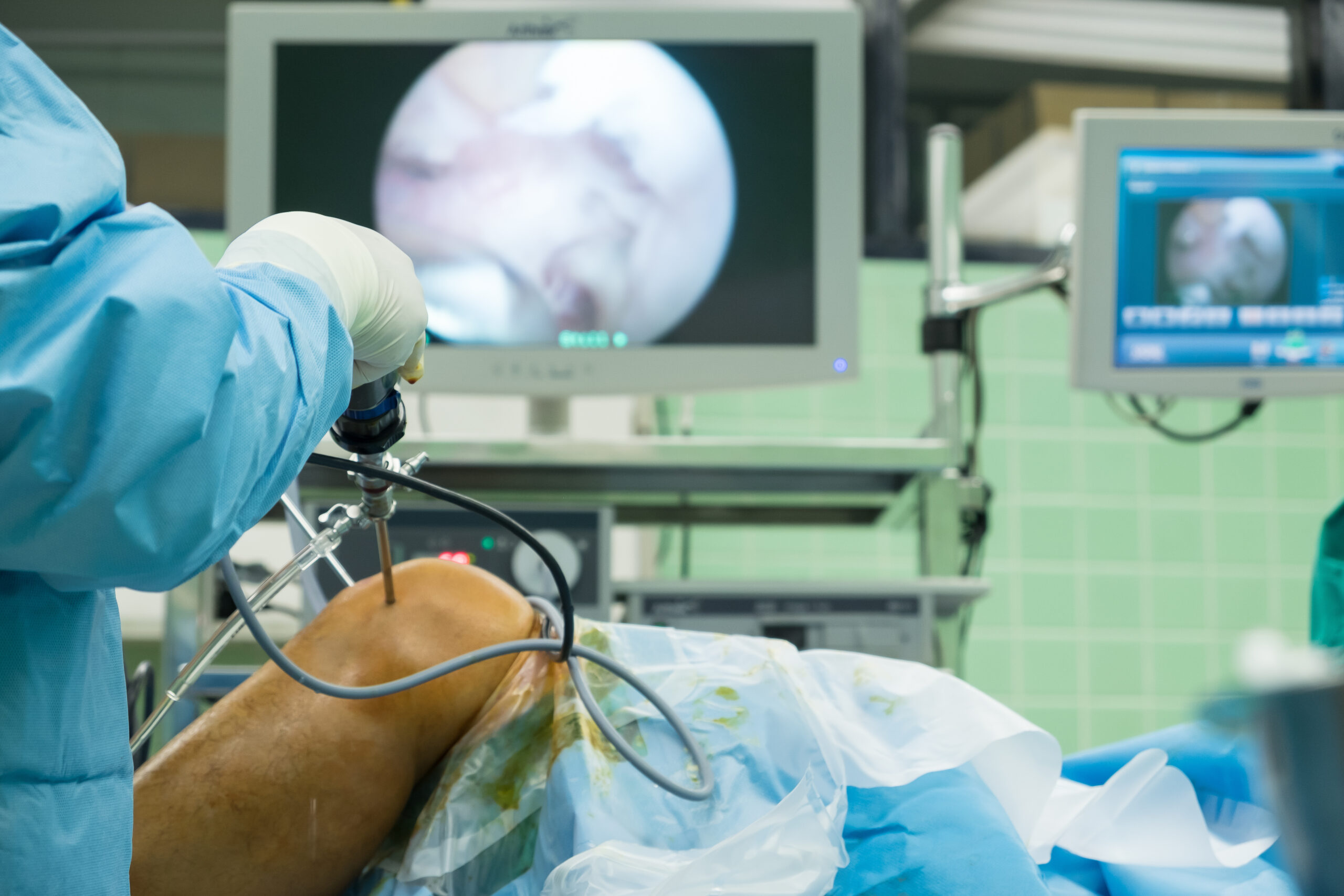
The administration’s recommendation to delay or cancel elective surgeries is a two-edged sword.
Recommendations made by the Centers for Medicare and Medicaid Services (CMS) on March 18 to delay elective surgeries have been implemented across the country according to circumstances and interpretation on a local level. Numbers of cases are projected to peak throughout April, May, and June, and in response, the American College of Surgeons (ACS) has released guidelines to triage elective surgeries to help inform decision making.
The cancellation policy has been suggested in order to mitigate the impact of the virus in the following ways:
- Minimize the spread of infection for both patients and providers. According to Kaiser Health News, a study out of China indicates that 41% of a group of 138 patients were infected during a hospital stay. Early numbers out of Italy indicated that 9% of those infected were healthcare workers.
- Keep facilities free to handle potential surges in critical care needs due to the pandemic. Hospitals in Spain are currently facing difficult decisions regarding their critical care patients. In the U.S., we’re working hard to avoid similar situations, though facilities in New York, Michigan, and Louisiana are already facing some equipment shortages. The U.S. Navy has sent hospital ships to help handle excess patients in New York and Los Angeles. In addition, other creative ideas have been suggested to help with patients if and when a surge occurs, such as using outpatient surgery centers, field hospitals, and public venues such as a shopping center in Memphis, Tennessee.
- Prioritize the use of PPE to ensure it’s available when needed. The U.S. is currently facing a PPE shortage, with some health systems already needing to reuse protective equipment or create their own. The CDC has had to “loosen the guidelines” regarding acceptable use due to the shortages.
The reasons for canceling or rescheduling non-urgent or elective procedures are clear and compelling, but as an unfortunate consequence, healthcare practices and hospitals will have to absorb the impact of this necessary step, and that can be painful.
Impact of Canceling Elective Surgeries
The United States is one of the largest markets for surgeries in the world, with over 129 million outpatient surgeries performed in 2018. Clearly, surgeries are an important source of revenue. Canceling elective procedures will create a financial burden for practices, physicians, and hospitals across the nation. As of March 31, 30 states have urged their healthcare systems to cancel elective surgeries in light of the pandemic.
 Consequently, many hospitals and medical practices are taking a huge financial hit. The reduced revenue due to surgery cancellations means healthcare facilities are having to make difficult decisions in their fight to remain operational. According to Business Insider, “Across the US, hospitals are slashing pay, laying off workers, reassigning people to other departments, or cutting hours.”
Consequently, many hospitals and medical practices are taking a huge financial hit. The reduced revenue due to surgery cancellations means healthcare facilities are having to make difficult decisions in their fight to remain operational. According to Business Insider, “Across the US, hospitals are slashing pay, laying off workers, reassigning people to other departments, or cutting hours.”
The decision to cancel, reschedule, or proceed as planned is not an easy one to make. Though three out of four hospitals across the nation are already seeing an impact, the 25% of hospitals that have not yet seen even a suspected case of the virus may have trouble justifying the loss of revenue. Some hospitals are continuing with routine surgeries amid protests from their staff who feel the risks are too high.
Some physician groups have shifted to outpatient surgery centers to minimize risk to patients and staff when possible, but many surgery centers are closed or have drastically cut back on procedures. The financial strain on the already struggling healthcare system, though not the greatest focus in light of the health of patients and staff, is a looming concern. Several options are in place to help medical practices and hospitals minimize the financial impact.
Three Ways to Get Financial Help
Paycheck Protection Program
The CARES Act signed into action on March 27 has temporarily expanded the traditional SBA loan and added a provision for loan forgiveness. According to sba.gov, “SBA will forgive loans if all employees are kept on payroll for eight weeks and the money is used for payroll, rent, mortgage interest, or utilities.”
Public Health and Social Services Emergency Fund
The fund was bumped from $2.9 billion to $100 billion when the CARES Act was put in motion in late March. The funds will be distributed through the Department of Health and Human Services, though it is unclear at this point exactly how the funds will be allocated.
Accelerated and Advanced Payments for Medicare
The CMS has expanded its accelerated and advance payments program for Medicare during the pandemic to a broader group of Medicare Part A providers and Medicare Part B suppliers. The advance payments can help with cash flow for those practices eligible for the program. The Fact Sheet released March 30, 2020, explains the program, the expansion, and how to apply.
The world-wide pandemic is wreaking havoc on our healthcare system, and we know each practitioner, medical practice, and hospital is facing difficult circumstances and impossible choices right now. We appreciate your efforts in keeping your communities safe. Please reach out to our customer support team if you have any communication needs we can assist with.